– AUGUST 2022 –
 How strokes impact vision loss and what you can do to help
How strokes impact vision loss and what you can do to help
Did you know that around a third of stroke survivors experience vision loss? When someone who has had a stroke loses sight in part of their visual field, this isn’t resulting from a problem with their eyes; it’s caused by a problem in their brain. This could occur anywhere along the course of the optic nerve, from the eyes themselves, to the primary visual cortex at the back of the brain in the occipital lobe.
One of the most common symptoms of visual field loss is called a hemianopia or quadrantanopia, which look like this:

- Complete hemianopia – is when half the is vision lost (on one side, either the left or right).
- Complete hemianopia with macular sparing – is when half the vision is lost (on one side, either the left or right), with a small amount of sparing or intact vision towards the middle of the face in the centre of the visual field (e.g. near the nose).
- Quadrantanopia – is when a quarter of the vision is lost.
The types of stroke that cause a hemianopia or quadrantanopia are: a large middle cerebral artery (MCA) infarct or haemorrhage affecting the deep brain structures; or a
posterior cerebral artery (PCA) infarct or occipital haemorrhage. An infarct is when a blood clot blocks an artery, whereas a haemorrhage is when there has been a bleed into the brain. Each artery supplies blood to a different area of the brain; if the blood supply gets blocked, that area of the brain dies.
The diagram below illustrates how the field of vision in the left and right eye is impacted, depending on where in the brain there has been a lesion (as indicated by the lightning bolts).
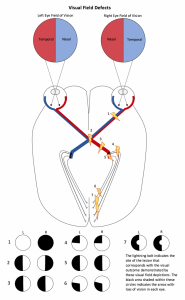
Things you need to know about vision loss from a stroke
- Stroke vision loss has nothing to do with the structures within the eyeball; it’s caused by damage to the optic nerve that transmits signals from the eye to the primary visual cortex.
- Loss of vision on the left side doesn’t mean the left eye isn’t working. Vision of the left side of your world comes from both of your eyes, as does the right.
- If sight doesn’t come back, there are ways to compensate for this, so that the person who has had a stroke can potentially still function independently. Our physiotherapists can help with this.
Strategies physios, carers and loved ones can do to help
- Remind the person to scan their environment to the affected side – e.g. if you turn your head far enough to the left then you can see the left side of your environment using the right side of your visual field.
- Slow things down, be more deliberate and cognisant of the black area to increase awareness and improve safety. For example, encouraging them to follow the frame of the door with their eyes to ensure they can judge it safely (in terms of where their body is spatially in relation to the door).
- Ensure supervision is given for community access, particularly with crossing the road, or in any unfamiliar environments or on unfamiliar surfaces that challenge balance. It will take time to learn to how to move safely again.
- Stand or sit on the affected side and encourage the person to turn their head and look towards you. Ask questions such as ‘how many fingers am I holding up?’, to see if they can see you.
There are many other types of stroke that affect vision in different ways, particularly those in the posterior fossa (cerebellum and brainstem). Our team are expertly trained to support people who have had a stroke, including if it has caused vision loss.
For free resources relating to how you can you help someone after having a stroke, this website has a wealth of useful information: https://enableme.org.au/
If you need to refer people in your care who require neuro physio, our dedicated specialists would be delighted to help. Contact us to book a free 15-minute consultation with our team here at Active Edge Physio. Alternatively, complete the referral form online and we’ll be in touch within 24 hours (on week days) to explore the best way forward.